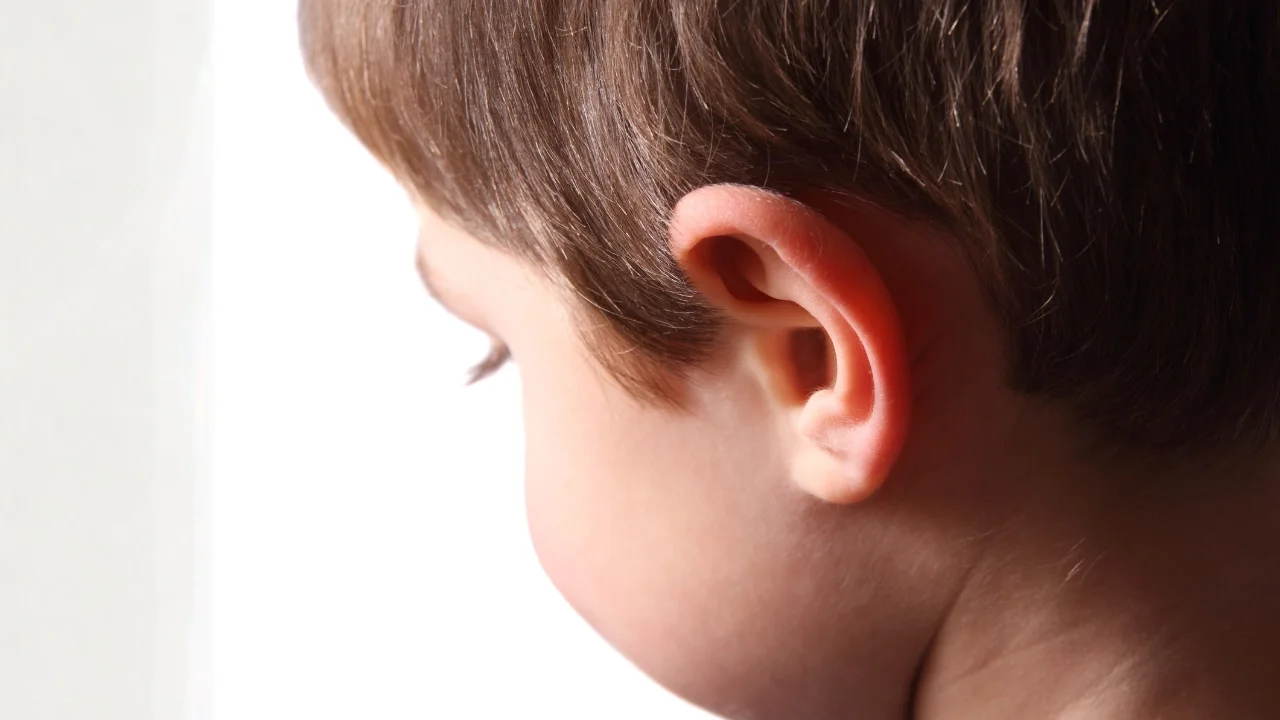
By R. Luke Sturgill, MD · Double Board-Certified Facial Plastic Surgeon · Carmel, Indiana
You want ears that don’t lead the conversation.
You don’t want ears that look “pinned.” You don’t want ears that look surgical. You want ears that simply—look like they belong.
Whether you’re an adult who’s spent years pulling hair forward, choosing angles in every photo, and quietly declining updos—or you’re a parent watching your child tug at their ears and shrink away from group pictures—you’re here because prominent ears have become a distraction from the person behind them.
Otoplasty corrects the shape, position, or proportion of the ears so they sit naturally against the head. It’s one of the most well-established procedures in facial plastic surgery—and when it’s done well, no one notices the ears at all. They just notice the person.
Double board-certified facial plastic surgeon in Carmel, Indiana. Dr. Sturgill’s practice focuses exclusively on the face and neck—which means even a procedure as straightforward as otoplasty gets the same precision, planning, and attention to facial proportion as every other surgery he performs.
The real question isn’t technique—it’s timing and candidacy.
Here’s the truth about otoplasty: the surgical technique itself is well-established. This isn’t a procedure where you need a surgeon who’s “reinvented” the approach. Cartilage is reshaped or repositioned, sutures hold it in place, and the ears sit closer to the head. Surgeons have been doing this successfully for decades.
So what actually separates a good outcome from a disappointing one? Judgment. Timing. Honest assessment of who should have the procedure—and when.
That’s where “Truth & Transparency” matters most—not because otoplasty needs a magic method, but because it needs honest answers to three questions:
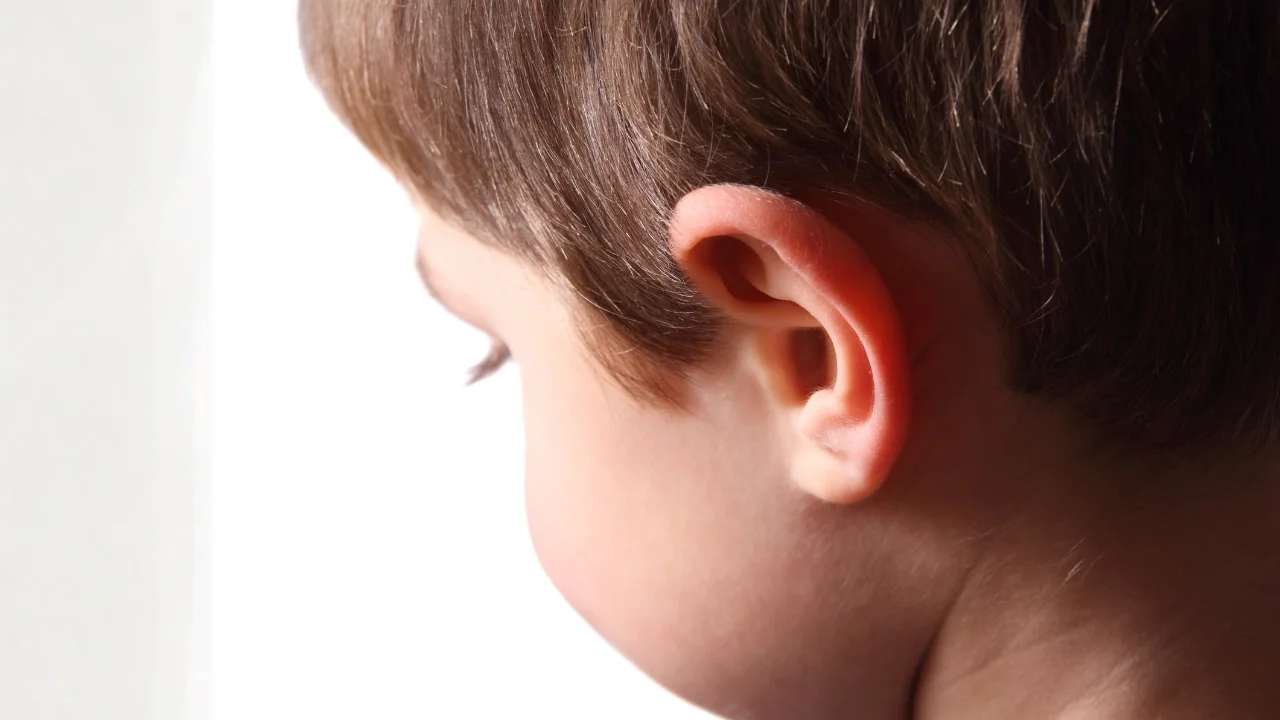
The right age and the right reason.
The minimum age for pediatric otoplasty is 7 years old. By age 5–6, the ear has reached approximately 90% of its adult size—so the anatomy is ready. But surgery isn’t just anatomy—it’s cooperation. A child needs to understand the headband, protect the ears during healing, communicate if something feels wrong, and handle a short-term change in routine without significant distress. That combination of physical readiness and emotional maturity typically converges around age 7.
But age alone doesn’t make a child a candidate.
If a child isn’t bothered by their ears, surgery is not the right move.
During every pediatric consultation, Dr. Sturgill speaks directly with the child. He wants to hear—from them—that their ears bother them. Is your child bringing it up on their own? Are they asking to fix it? Are they avoiding certain hairstyles, activities, or situations because they feel self-conscious?
Parents can notice a problem first—and that’s normal. But the healthiest long-term outcomes happen when the child is doing this for themselves, not to satisfy someone else’s standard. A parent who notices prominent ears and a child who is genuinely distressed by them are two different situations. If a 7-year-old is unbothered and it’s only Mom or Dad who’s worried, Dr. Sturgill will say so honestly. Surgery for a child who doesn’t want it isn’t good surgery—it’s unnecessary surgery.

It’s never too late.
Many adults assume otoplasty is “only for kids.” It’s not. There is no upper age limit.
Adults pursue ear correction for the same reasons—they’ve simply been living with it longer. Years of keeping hair down even when they’d prefer it up, avoiding windy situations and swimming, feeling self-conscious on video calls, or quietly managing prominent ears through strategic positioning in every photo.
If this has bothered you for 20 or 30 years, that’s not a trivial concern—it’s a long-standing one. You’re not behind. You’re just ready now.
Adult cartilage is slightly stiffer than in children, which actually provides some advantages for maintaining the correction long-term.
The procedure, recovery, and outcomes for adults are excellent. Some of the most grateful patients are adults who finally address something that’s quietly bothered them for decades.
What Dr. Sturgill is evaluating.
Even a “straightforward” procedure requires careful diagnosis—because the reason an ear is prominent isn’t always the same, and the surgical approach depends entirely on what’s actually causing it.
During your consultation, here’s what Dr. Sturgill is assessing:
The Anatomical Source of Prominence
Prominent ears typically result from one or both of the following:
Different causes require different adjustments. Treating the wrong issue—or treating only one when both are present—can produce an ear that looks “pinned” or unnatural. Getting the diagnosis right is what makes the result look like it was always that way.
Asymmetry
Almost no one has perfectly symmetrical ears—and you’d be surprised how common meaningful asymmetry is. Each ear is evaluated independently. The goal is balanced improvement and natural harmony, not mathematical perfection.
Cartilage Strength and Skin Quality
Cartilage varies significantly by age and individual. In children, softer cartilage is an advantage during reshaping but requires careful suture technique to maintain correction long-term. In adults, firmer cartilage sometimes demands more deliberate sculpting. Skin thickness and elasticity also affect how the ear will hold its new shape over time.
Expectations and Emotional Readiness
Especially for pediatric patients: does the child understand what surgery is and why they want it? For adults: are you looking for natural repositioning, or chasing perfection? The evaluation determines the plan—and the details are different for every patient.

See the difference for yourself.
Dr. Sturgill shares patient photos only with explicit consent. The goal of otoplasty is a result so natural that no one notices the ears at all—they simply stop being a distraction. That subtlety is the point.

Individual results may vary. Photos shown with patient consent.
The procedure.
Otoplasty is designed to reposition and reshape the ear so it sits closer to the head in a natural, unoperated way.
Hidden in a natural crease
Behind the ear, in the natural crease where the ear meets the head. Once healed, the scar is virtually invisible—even with short hair or ears fully exposed. This is one of the most favorable scar locations in all of plastic surgery.
Cartilage reshaping with precision
Through the incision, cartilage is reshaped, scored, or supported with permanent internal sutures to create a more natural fold and reduce prominence. In some cases, a small amount of excess cartilage or skin is removed.
The specific approach depends on what’s driving the prominence—conchal reduction, antihelical fold creation, or both.
Tailored to the patient
1–2 hours
Depending on complexity and whether one or both ears are addressed.
Private, accredited surgical facility
Outpatient procedure at Meridian Plastic Surgery Center, our private AAAHC-accredited surgical facility. Home the same day. No overnight stay. No drains.
The goal is not ears that look tight, flat, or artificially pressed against the head. The goal is ears that look like they were always that way. That’s the entire point.
Recovery — what to expect.
Otoplasty is one of the more straightforward recoveries in facial plastic surgery. Discomfort is typically mild, bruising is minimal, and most patients—children and adults alike—are surprised by how quickly they return to normal activity.
Here’s the general recovery timeline:
Most patients describe the recovery as easier than expected. Children, in particular, tend to bounce back quickly—and the excitement of seeing their ears sit differently for the first time is its own kind of motivation.
A note for parents: children do remarkably well with this procedure. They are often less anxious about the recovery than their parents are. If your child has been asking for this surgery, they’re usually thrilled to trade a week with a headband for ears that no longer bother them.
We provide detailed post-operative instructions at your pre-surgical appointment and are available by phone or text throughout your recovery. No question is too small.

Procedures often considered alongside otoplasty.
Otoplasty is frequently performed as a standalone procedure. But for patients already planning surgery, combining it with another procedure can address multiple concerns under one anesthetic—reducing total downtime and overall cost.
Rhinoplasty
The most common combination with otoplasty. Patients addressing facial proportion often find that refining the nose and repositioning the ears together produces a more balanced result than either procedure alone. Both heal independently and don’t interfere with each other’s recovery.
Brow Lift
For adult patients seeking upper facial rejuvenation, an endoscopic brow lift can be performed in the same session as otoplasty. The incisions are completely separate, the recovery timelines overlap, and the combined result addresses the full upper third of the face.
Earlobe Repair
Torn, stretched, or elongated earlobes from earrings or aging can be corrected at the same time as otoplasty. If you’re already addressing the ears, it makes sense to handle everything in one procedure rather than scheduling a second surgery later.
Extended Deep Plane Face and Neck Lift
For adult patients already planning facial rejuvenation, otoplasty can be performed in the same session as a deep plane facelift. The incisions are in close proximity, recovery timelines overlap, and addressing both at once avoids a second anesthetic and a second round of downtime.
Whether you’re considering otoplasty alone or as part of a broader plan, every combination is evaluated individually during your consultation. Dr. Sturgill will only recommend combining procedures when it’s safe, practical, and genuinely beneficial for the patient.
Why Patients Choose
Dr. Sturgill
Patients travel from across the country for care that prioritizes honesty, artistry, and results that look like you.

Specialization
Double board-certified in facial plastic surgery. He focuses exclusively on the face and neck — performing otoplasty at a volume that ensures consistency and mastery.
Truth & Transparency
No sales pressure. No "magic" wands. Just honest assessments of what anatomy and surgery can achieve — so you can make decisions with clarity, not confusion.
The "Unoperated" Look
His aesthetic goal is for you to look like yourself — just rested, refined, and restored. Never overdone, never obvious.
What Patients Are Saying About Dr. Sturgill
Real reviews from real patients—because the best referral is an honest one.
Ready to take the next step?
Your consultation is a planning session — not a sales pitch.
Dr. Sturgill will evaluate your facial anatomy, discuss your goals, and give you an honest assessment of what surgery can — and cannot — achieve. You will leave with a clear understanding of whether this procedure is right for you.
What to expect
- Review your concerns and goals in detail
- Receive a facial analysis with a personalized surgical plan
- See before-and-after photos of what YOU will look like after surgery
- Have all your questions answered directly
Consultations typically last around 45 minutes.
Book Your Consultation
Your Questions, Answered
-
Dr. Sturgill performs otoplasty on children starting at age 7. By this age, the ears have reached approximately 90% of their adult size, meaning the cartilage is developed enough to reshape predictably and hold its new position. Just as importantly, most 7-year-olds are mature enough to understand the procedure, cooperate with post-operative instructions—like wearing the protective headband and avoiding rough play—and participate meaningfully in the decision.
Younger than 7, and the combination of softer cartilage and limited cooperation with recovery typically makes the timing premature.
-
The most important indicator isn’t the parent’s concern—it’s the child’s. Dr. Sturgill wants to see that the child is the one who’s bothered by their ears. That might look like them bringing it up on their own, refusing to wear hair up, covering their ears in photos, or telling you what other kids have said.
If your child has never mentioned it and the concern is primarily yours, Dr. Sturgill will be straightforward about whether surgery is appropriate at this time. The ideal candidate is a child who is aware of the issue, bothered by it, and willing to go through the recovery process. Surgery should support a child’s confidence—not replace it.
-
The incision is placed behind the ear, in the natural crease where the ear meets the head. Once fully healed, the scar is virtually invisible—even with short hair, a buzzcut, or ears fully exposed. This is one of the most favorable scar locations in all of plastic surgery.
Nothing in surgery is truly “scar-free,” but in otoplasty, the scar is generally not noticeable in everyday life.
-
Recovery from otoplasty is relatively straightforward:
- Days 1–3: Mild to moderate soreness and swelling. A soft, protective headband is worn continuously to keep the ears supported in their new position.
- Days 5–7: Most children return to school; most adults return to work. Swelling and bruising (if any) are usually minimal at this point.
- Weeks 1–6: The headband transitions to nighttime wear only—protecting the ears during sleep when accidental bending is most likely. No contact sports, roughhousing, or activities that risk hitting or bending the ears for approximately 6 weeks.
- Long-term: Final results are visible once all swelling resolves—typically within 2–3 months—though most of the improvement is apparent within the first couple of weeks.
The headband is the single most important part of recovery. It protects the correction while the cartilage heals in its new position.
-
Honest answer: there is a small recurrence risk with any otoplasty—typically quoted in the literature at around 5–10%, though the degree of recurrence varies. In most cases, if there’s any relapse, it’s partial and subtle rather than a full return to the original position. Cartilage has “memory” and can sometimes try to reassert its original shape.
Using permanent sutures, appropriate cartilage reshaping, and ensuring good compliance with the headband during recovery all minimize this risk. Dr. Sturgill discusses this candidly during consultation—no procedure has a 100% guarantee, and you deserve a surgeon who tells you that upfront rather than promising perfection. If meaningful recurrence occurs, a minor revision can address it.
-
Less than most people expect.
For children: They’re under general anesthesia during the procedure and feel nothing. Post-operatively, most kids describe mild soreness—not sharp pain—which is well-managed with over-the-counter medication like Children’s Tylenol for the first few days.
For adults: Under IV sedation or general anesthesia, you’ll feel nothing during the procedure itself. Post-operative discomfort is similar—a dull ache and tightness for a few days, easily managed without narcotic medication in most cases.
The ears may feel tight or “weird” as swelling settles, but significant pain is uncommon. The most annoying part for many patients is simply wearing the headband.
-
Absolutely. There is no upper age limit. Many of Dr. Sturgill’s adult otoplasty patients are in their 30s, 40s, or older—people who’ve quietly managed prominent ears their entire lives through hairstyle choices, hat-wearing, or simply avoiding certain situations.
Adult cartilage is stiffer than in children, which actually provides some advantages for maintaining the correction long-term. The procedure, recovery, and outcomes for adults are excellent—and it’s one of the most straightforward ways to resolve something that may have been a source of self-consciousness for decades.
-
Otoplasty is cosmetic reshaping and repositioning of an ear that is fully formed but prominent, asymmetrical, or disproportionate. The ear’s basic structure is all there—it just needs to be refined.
Ear reconstruction is a different category of surgery entirely. It addresses ears that are absent, severely underdeveloped (microtia), or damaged by trauma. Reconstruction typically involves building or rebuilding the ear framework—often using rib cartilage grafts—and is a more complex, multi-stage process.
If your child has microtia or a congenital ear deformity beyond simple prominence, Dr. Sturgill can evaluate the situation and, if it falls outside his scope, refer you to a specialist who focuses specifically on ear reconstruction.
-
In most cases, no. Otoplasty is classified as a cosmetic procedure by the majority of insurance carriers, which means it’s typically an out-of-pocket expense. This applies to both children and adults.
There are rare exceptions—some plans may offer partial coverage for pediatric patients if prominent ears are documented as causing significant psychological impact, but this is uncommon and varies widely. Dr. Sturgill’s office can provide you with the necessary documentation if you’d like to submit a pre-authorization request, but it’s best to plan on self-pay. Financing options are available.

